Functional rhinoplasty in Turkey is a surgical procedure designed to correct structural nasal problems that impair breathing while preserving or improving nasal anatomy. The operation focuses on repairing the septum, nasal valves, and internal support structures to restore healthy airflow and stable nasal function.
Cost and medical standards of functional rhinoplasty in Turkey are widely recognized for combining advanced surgical technology with internationally accredited hospitals. Experienced ENT and facial plastic surgeons perform detailed anatomical evaluations and individualized surgical planning to address airway obstruction and structural deformities.
Recovery process after functional rhinoplasty in Turkey generally involves a short hospital stay, controlled postoperative care, and gradual improvement in nasal airflow. Swelling and mild congestion decrease within weeks, while internal tissues continue healing over several months, allowing the nasal passages to regain stable respiratory function.
Choosing a qualified ENT or facial plastic surgeon in Turkey for functional rhinoplasty ensures accurate diagnosis and safe surgical correction of nasal obstruction. Board-certified specialists use modern imaging, functional assessments, and refined surgical techniques to protect nasal support structures and maintain long-term breathing quality.

Prof. Dr. Fehmi Döner
ENT and Head & Neck Surgery Specialist
I completed my primary and secondary education in İzmir. I completed my medical education at Istanbul University Cerrahpaşa Faculty of Medicine in 1988. I received my specialization training at Atatürk University Faculty of Medicine, Department of Otorhinolaryngology. During my specialization training, in order to increase my knowledge and experience, I spent different periods of time at Istanbul University Istanbul Faculty of Medicine, Department of Otorhinolaryngology, and participated in clinical studies.
After receiving my specialization in 1994, I worked at Kütahya State Hospital for eight months, and then in December 1994, I was appointed as an assistant professor to the Department of Otorhinolaryngology at Süleyman Demirel University.
View MoreIs Our Nose Only About Appearance, or Is It a Complex Machine?
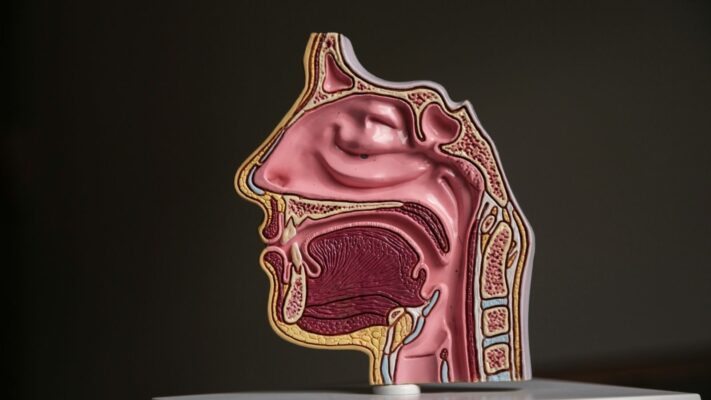
You should think of your nose as much more than an aesthetic organ sitting right in the middle of your face, but as an advanced “air-conditioning system” at the entrance of your body. The air you inhale from outside is often different from body temperature, dry, and full of particles. In a very short fraction of a second, your nose warms, humidifies, filters, and makes this air suitable for your lungs to use as efficiently as possible. The functioning of this system is not like a simple pipeline; inside, there is an aerodynamic structure in which complex laws of physics such as the Bernoulli principle and Poiseuille’s law operate:
A millimetric narrowing in the airway or an anatomical disorder disrupts this delicate balance. This does not only create the feeling of “my nose is blocked”; it directly affects your sleep quality, your energy level during the day, your sports performance, and even your heart health. In functional rhinoplasty, our main goal is not only to create a nose that looks beautiful from the outside, but also to ensure that the gears of this physiological factory turn flawlessly. No matter how beautiful a building’s facade is, if its ventilation system does not work, living in that building is uncomfortable. The same is true for the nose. In this context, the tasks of the nose are as follows:
- Warming
- Humidifying
- Filtering
- Smelling
- Voice resonance
What Is Septal Deviation, the Main Culprit Behind Nasal Congestion, and How Is It Corrected?
A large majority of our patients apply with complaints of chronic nasal congestion as well as aesthetic concerns. The most common anatomical cause of this congestion is the curvature of the wall we call the “septum,” which divides the nasal cavity into two corridors, right and left. In ideal anatomy, this wall is expected to be exactly in the middle, in a perfectly straight line. However, as a result of genetic factors, birth traumas, or impacts received later, the septal cartilage may bend to the right or left and form S- or C-shaped curves. We call this “septal deviation.”
Septal curvature mechanically narrows the airway. But the problem is not only that air cannot pass through. On the narrowed side, airflow speeds up and turbulence occurs, which can lead to dryness, crusting, and, over time, bleeding in the nasal tissues. On the other side, that is, in the wider canal, the body tries to restore balance by enlarging the turbinates (conchae) to fill that space. In other words, with bone curvature on one side and turbinate enlargement on the other, both channels become blocked. The most common symptoms of septal deviation are as follows:
- Unilateral nasal congestion
- Sleeping with the mouth open
- Snoring
- Frequently recurring sinusitis
- Nosebleeds
- Facial pain
- Postnasal drip
The septoplasty procedure we perform to solve this problem, contrary to popular belief, is not just an internal correction. The septum is like the main column that carries the roof of the nose. While correcting this column, it is vital not to lose the support of the external nasal framework. In modern surgery, while correcting the septum, we prefer to reshape the curved cartilages and use them as proper support material instead of removing and discarding them. In this way, the airway is opened and a solid foundation is created for both the nasal tip and the dorsum.
Why Do the Wings of Your Nose Collapse Inward When You Take a Deep Breath?
Some of our patients come with the complaint, “I don’t have a crooked nasal bone, but I still can’t breathe deeply; when I inhale, the sides of my nose close.” Here, a very critical mechanism called the “nasal valve” comes into play. The nasal valves are the areas where the nasal airway is narrowest and airflow resistance is highest. These regions, divided into internal and external valves, must resist the negative pressure that occurs during inhalation.
If the cartilages in your nasal wings are weak or the angle between the nasal roof and the septum is too narrow, with the vacuum effect created when you take a deep breath, the nasal wings adhere inward. Just like a weak straw collapsing when you try to drink a thick beverage through it. We call this “dynamic collapse.” This condition seriously bothers the patient, especially when doing sports or exerting effort.
In functional rhinoplasty, to correct this, we need to make the “open-door policy” permanent. We strengthen these weak areas with special grafts (support pieces) prepared from the patient’s own cartilage. These grafts act like the poles of a tent, widening the airway and preventing the wings from collapsing during breathing. Thus, no matter how deeply the patient breathes, the airway remains open and stable.
Why Do the Turbinates Enlarge, and How Should They Be Treated?
Another important actor in nasal congestion is the turbinates. These structures on the lateral walls of the nose are very rich in blood vessels and are responsible for warming and humidifying the air. However, due to allergic reactions, air pollution, smoking, or septal curvature, these turbinates can swell excessively (hypertrophy).
In older surgeries, these turbinates were sometimes completely cut out and removed. But as medicine advanced, we saw that completely removing them leads to a much more serious problem called “Empty Nose Syndrome,” in which the patient feels unable to breathe even though the nose is open, and the inside of the nose becomes dry and crusted. Because the air, unprocessed, dry and cold, hits the nasopharynx directly. The factors that trigger turbinate enlargement are as follows:
- Allergic rhinitis
- Air pollution
- Smoking
- Hormonal changes
- Long-term nasal spray dependence
- Septal deviation
Today, the modern approach we adopt is “tissue-preserving” surgery. Using technologies such as radiofrequency or microdebrider, we reduce only the inside of the turbinate without damaging the valuable mucosal layer on its surface that humidifies the air. You can think of it like hollowing out an orange without damaging its peel. Thus, while the turbinate decreases in volume and opens the airway, it continues to perform its warming and humidifying function.
How Do We Decide on the Surgical Technique: Open or Closed?
When rhinoplasty is mentioned, one of the first questions that comes to patients’ minds is about the technique: “Doctor, will you do it open or closed?” In fact, these two techniques are not rivals, but different keys in the surgeon’s hand for solving different problems. When deciding, the patient’s anatomy, the complexity of the problem, and the targeted change are decisive.
The open technique is based on the principle of lifting the nasal skin with a very small incision made in the area between the two nostrils called the columella. This method gives us the chance to see the entire skeletal structure of the nose, the cartilages, and the bones with the naked eye, in their natural positions. Especially in cases with severe deviations, in patients who have had previous surgery (revision), or in complex cases requiring millimetric suture techniques and grafting at the nasal tip, the open technique provides us with “visual control.” As a surgeon, I can fix everything in exactly the place I want by seeing it.
The closed technique is the method in which all incisions are made inside the nostrils and there is no scar outside. Its biggest advantage is that, since the skin is not completely separated from the bone and cartilage framework, the lymphatic circulation and ligaments at the nasal tip are better preserved. This means less swelling after surgery and a slightly faster recovery process. Thanks to the endoscopic instruments and visualization techniques that have developed today, quite detailed problems can also be solved with the closed method. However, which method will be used depends entirely on what the patient’s nose needs. What matters is not the technique, but whether that technique can solve the problem in your nose.
Is It Possible to Preserve the Natural Structure of the Nose?
In traditional rhinoplasty, to correct the nasal hump, the upper roof of the nose was usually rasped or cut and removed. This could sometimes lead to disruption of the natural anatomical integrity of the nose and an “open roof” deformity. The philosophy of “Preservation Rhinoplasty,” which has become popular in recent years and which we also frequently use, has completely changed this approach.
In preservation rhinoplasty, we do not touch the natural bone and cartilage integrity on the dorsum of the nose. Instead of demolishing the roof to correct a humped nose, we lower the nose as a whole by removing thin strips from the base of the nose (Letdown) or push it inward (Pushdown). The biggest advantage of this technique is that the natural light reflections, curves, and texture of the nasal dorsum are not disrupted. Also, since the nasal roof is not opened, the risk of airway problems decreases and the recovery process is much more comfortable. This may not be suitable for every patient, but in suitable cases it is a very valuable approach that allows us to achieve “natural results as if no surgery was done.”
Is the Era of Breaking and Shattering Over? What Is the Difference of Piezo Surgery?
One of the greatest gifts of technology to surgery is undoubtedly “Piezo,” that is, ultrasonic bone shaping devices. In the past, hammers, chisels, and rasps used to shape the nasal bones could cause some trauma to the soft tissue, vessels, and nerves around the bone, no matter how carefully they were used. This led to the feared appearance of “bruised eyes and a swollen face” after surgery.
Piezo technology, on the other hand, works with sound waves (ultrasonic vibrations). The most important feature of this device is that it is “tissue-selective.” That is, it only cuts or shapes hard tissue (bone); when it touches the skin, mucosa, or vessels, it stops and does not harm them. In this way, we can cut and shape bones with millimetric precision, as if drawing with a pencil, without “breaking” them. As a result, our patients have much less bruising and swelling, the recovery process speeds up, and the healing of the bones occurs much more controlled. Piezo is a revolution that increases surgical predictability and maximizes patient comfort. The main advantages offered by Piezo surgery are as follows:
- Less bruising
- Less swelling
- Faster recovery
- Millimetric bone shaping
- Prevention of soft tissue damage
- More natural nasal dorsum transitions
What Is “Biomechanical Support” That Prevents Nasal Collapse?
One of the biggest fears in functional rhinoplasty is that the nose may collapse or droop over time. The nasal framework must be strong enough to carry the weight of the skin on it and the negative pressure created during breathing. If too much tissue is removed from this framework, the nose that initially looks good begins to collapse over months or years and breathing problems recur.
For this reason, in modern surgery we follow a “structuring” rather than a “reductive” approach. We strengthen the weak points of the nose, especially with your own cartilage obtained from the septum.
The main types of grafts we use are as follows:
- Spreader Grafts
- Columellar Strut
- Alar Batten Grafts
- Rim Grafts
Although these procedures give the nose a slightly more complex architecture, in the long term they enable us to obtain a nose that maintains its form, does not deform with age, and always breathes. Spreader grafts work like beams placed in the middle vault of the nose; they widen the airway and prevent collapse of the middle vault. The columellar strut is a pole-like cartilage we place at the nasal tip; it prevents the nasal tip from sagging over time by yielding to gravity. While alar batten grafts support the nasal wings and prevent them from closing during breathing, rim grafts are thin cartilages placed along the edges of the nostrils that both provide symmetry and strengthen the alar margins.
Get in Touch!
What Awaits You Before Surgery?
The foundation of a successful result is laid with a detailed analysis. While examining you, we do not just look from the outside and say, “let’s lift this, lower that.” With endoscopic cameras, we go into the deepest points of the nose and check whether there is a hidden deviation, polyp, or adenoid tissue in the back. Most of the time, by requesting Computed Tomography (CT)
we examine the condition of the sinuses, the thickness of the bony structures, and anatomical variations three-dimensionally.
We also take your photographs from certain angles in a professional studio environment. The simulation studies we perform on these photographs are very valuable both for understanding your expectations and for showing you what is and is not surgically possible. Even the thickness of your skin changes our surgical plan; while we need to build a stronger framework in a thick-skinned patient, in a thin-skinned patient we need to camouflage the edges of the grafts much better. The preparations made in the preoperative process are as follows:
- Detailed physical examination
- Endoscopic intranasal examination
- Paranasal sinus tomography
- Photography and analysis
- Blood tests
- Anesthesia consultation
- Simulation study
Recovery Process: What Are the Myths and the Facts?
The recovery process after rhinoplasty is one of the processes that patients fear the most but that passes most comfortably with modern techniques. To the question “Will I have a lot of pain?” I usually answer, “No; rather than pain, you will feel a sense of fullness and pressure in the first days.” If we consider the process day by day, you can actually see that there is nothing to be afraid of.
In the first 48–72 hours, it is natural to have some swelling even if we use Piezo. By keeping the head elevated and applying regular ice, we get through this process with minimal swelling. Thanks to silicone splints, the stories of suffering while removing tampons are now history; you can breathe through the channels inside these silicone splints.
Generally, on the 7th day we remove the splint on the nose and any stitches if present. This is the moment you first meet your new nose. Even if you have swelling, you notice the big change. You can return to your social life or work at this point. In the first month, most of the swelling has subsided. You can start light sports such as walking. However, it is very important to protect your nose from impacts. For the nose to take its final shape, for the skin to settle completely on the bone and cartilage framework, it can take from 6 months to 1 year depending on skin thickness. This is a process of patience.
Things to pay attention to during the recovery process are as follows:
- Keeping the head elevated
- Regular ice application
- Reducing salt consumption
- Avoiding eyeglass use
- Staying away from heavy exercise
- Protection from the sun
- Intranasal moisturization
Not smoking is also one of the most critical points of this process; because smoking constricts the capillaries that nourish the tissues and both delays wound healing and increases the risk of infection.
How Does This Surgery Transform Your Quality of Life?
It is insufficient to see functional rhinoplasty only as a beauty surgery. This operation is a point of starting life anew for many patients. A person who begins to breathe comfortably through the nose has improved sleep quality; they wake up in the morning more refreshed, without headaches, and with a throat that is not dry. Increased oxygen saturation improves the ability to focus and mental clarity during the day. Problems such as getting tired quickly and becoming short of breath during exercise disappear.
Along with all of this, the self-confidence of an individual who feels better when looking in the mirror and is at peace with their face also increases. They behave more comfortably in social relationships and express themselves better. In the scientific studies and surveys we conduct, we see that patients’ functional and aesthetic satisfaction increase dramatically in the postoperative period.