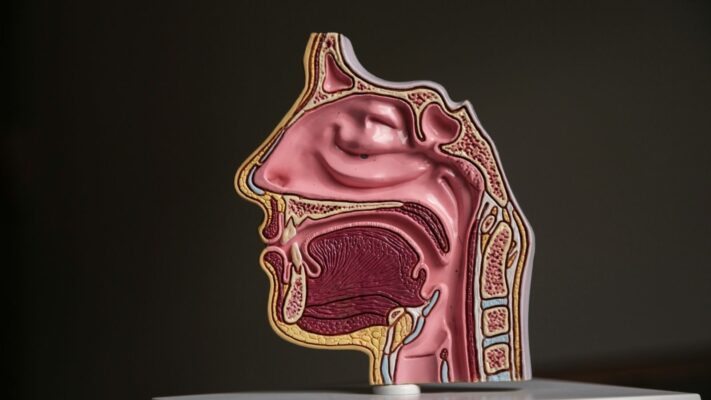
Nose reduction surgery in Turkey is a cosmetic surgical procedure that decreases the size of the nose by reshaping bone and cartilage to achieve balanced facial proportions. The operation is performed by qualified plastic surgeons and focuses on reducing nasal width, hump prominence, or overall nasal volume while preserving natural breathing function.
Rhinoplasty procedures for reducing nose size in Turkey are commonly performed using advanced surgical planning and precise cartilage modification techniques. Surgeons evaluate facial symmetry, nasal structure, and skin thickness to design individualized treatment plans that deliver proportionate, natural-appearing results with stable long-term outcomes.
Cost advantages and medical tourism infrastructure in Turkey make nose reduction surgery a widely preferred option for international patients. Accredited hospitals, experienced rhinoplasty specialists, and comprehensive postoperative care programs contribute to safe procedures, predictable recovery timelines, and consistently high patient satisfaction rates.
Recovery process after nose reduction surgery in Turkey generally involves short hospital observation, controlled swelling management, and gradual nasal shape stabilization over several weeks. Patients typically resume routine daily activities within a limited period while final aesthetic refinement continues as tissues heal and adapt.

Prof. Dr. Fehmi Döner
ENT and Head & Neck Surgery Specialist
I completed my primary and secondary education in İzmir. I completed my medical education at Istanbul University Cerrahpaşa Faculty of Medicine in 1988. I received my specialization training at Atatürk University Faculty of Medicine, Department of Otorhinolaryngology. During my specialization training, in order to increase my knowledge and experience, I spent different periods of time at Istanbul University Istanbul Faculty of Medicine, Department of Otorhinolaryngology, and participated in clinical studies.
After receiving my specialization in 1994, I worked at Kütahya State Hospital for eight months, and then in December 1994, I was appointed as an assistant professor to the Department of Otorhinolaryngology at Süleyman Demirel University.
View MoreHow Is Facial Analysis Performed Before Nose Reduction Surgery?
Behind every successful surgery lies detailed planning done in the examination room long before the operating theater. When I see you in front of me, the first thing I look at is not only the hump of your nose or the tip. The width of your forehead, the prominence of your cheekbones, your lip structure, and most importantly the position of your chin, can completely change the plan we will make. We call this “facial mapping.”
The nose is not an island independent of the other parts of the face. For example, in a patient with a retruded chin, the nose is perceived as much larger and more projected than it actually is. In such a case, reducing the nose alone may not be enough; perhaps a small adjustment to the chin could completely change the perception of the nose and create a much more natural profile. We divide your face vertically and horizontally into certain segments and look at the ratios of these segments to one another. The concept known as the golden ratio comes into play exactly here.
Gender is also very critical in planning. In women, having a slightly wider angle between the nose and the lip—meaning a mildly upturned nasal tip—provides a fresher, more feminine, and youthful expression. In men, this angle should be steeper and the tip should not be overly upturned, because preserving sharp and masculine facial lines is essential. The main structures we examine in the preoperative analysis are:
- Forehead width
- Brow structure
- Cheekbones
- Lip distance
- Chin tip
- Neck angle
Why Is Skin Thickness Important in Nose Reduction?
This is the factor that surprises my patients the most, yet affects the success of the result the most: your skin structure. No matter how perfectly I shape the bones and cartilage inside, the “cover,” meaning your skin, is like the ultimate boss that determines how the result will reflect outward:
Explaining this with the example of a bed and the cover spread over it is always clearer. If you spread a very thick, woolen quilt over the bed, you cannot see the fine details, corners, or patterns underneath. Thick-skinned noses are like that. Thick and oily skin tends to mask the elegant curves, subtle transitions, and sharp lines we create underneath. Therefore, in thick-skinned patients, we have to make our surgical techniques a bit more pronounced and defined so that the shape underneath can be seen once the thick skin drapes over it.
The opposite—very thin skin—is like a silk sheet. It reflects everything underneath exactly as it is. While this may seem like a great thing, it is actually a major challenge for the surgeon. Because a millimetric irregularity left on the bone, a tiny asymmetry, or an unevenness becomes immediately visible under thin skin. For this reason, in thin-skinned patients, we use what we call “camouflage techniques,” methods in which we smooth the surface by laying special tissues under the skin.
Another effect of skin thickness is on the healing time. Thick skin, by its nature, retains more fluid and is prone to swelling. For this skin to adhere to the reduced framework we create and for the nose to take its final shape may take 1.5, sometimes even 2 years. In thin-skinned patients, this process is much faster. The criteria we assess when analyzing your skin structure are:
- Pore size
- Oiliness level
- Skin elasticity
- Color tone
- Vascular pattern
Can Breathing Problems Be Corrected with Rhinoplasty?
As an ENT specialist, I have an unchanging rule: A nose that cannot breathe is a failure, even if it is the most beautiful nose in the world. A very large proportion of patients who want rhinoplasty already have breathing problems, whether they are aware of them or not. Many patients are not even aware that they have been breathing poorly because they have become used to it over the years.
When we say nose reduction surgery, technically we are narrowing the overall volume of the nose. If we only reduce the outside without widening the airway inside, the patient can end up with a nose that feels pinched, unable to breathe. That is why aesthetic surgery and functional surgery are an inseparable whole. While improving the outside, we also address the internal problems in the same session.
The most common problem we encounter is “septal deviation,” the curvature of the wall that divides the nose into two halves. Correcting this wall is like killing two birds with one stone for us. We open the airway for the patient and we also do not discard the cartilage we remove from the deviated parts; we use it as “spare parts” to shape the nasal tip or to strengthen the dorsum.
Another important issue is the nasal turbinates. These structures, medically called “conchae,” can swell due to allergies or structural reasons and block the airway. During surgery, we can shrink these turbinates using modern technologies such as radiofrequency, widening the air corridor. In other words, when you wake up, you should have a nose that not only looks better but also allows your lungs to fill with oxygen comfortably. The main factors that hinder breathing are:
- Septal deviation
- Enlarged turbinates
- Nasal valve narrowing
- Presence of polyps
- Chronic sinusitis
Do Preoperative Simulations Reflect Reality?
One of the greatest opportunities technology offers us is 3D design and simulations performed before surgery. When we take your photograph during the examination and project it onto the computer screen and start making adjustments, we are actually establishing a language of communication. When you say “let it be curved,” we clarify what you mean, and when I say “let it be natural,” we clarify what I plan—through these visuals.
However, there is a very fine line here, and I emphasize it especially to every patient: This is not a “guarantee of outcome” document; it is a “goal-setting” study. There is a world of difference between deleting or shaping pixels on a screen and shaping living tissue, bone, and cartilage. Even if I place the cartilages millimetrically during surgery, the body’s response during healing, your wound-healing speed, and your skin thickness will affect the result.
Still, planning performed by experienced hands gives an idea that is close to reality by about 90–95%. Thanks to these simulations, we prevent disappointments. For example, you have the chance to see something we cannot do or that would not suit your face and say, “No, that’s not for me.” This work is the strongest tool that allows the patient and the physician to speak the same aesthetic language.
What Are the Differences Between Open and Closed Rhinoplasty?
Let’s address the question “Open technique or closed technique?”—a topic frequently debated in the rhinoplasty world and one that confuses patients. In fact, these two methods are like entering the same house through different doors. The renovation we do inside the house is the same; only our entry route changes.
In closed rhinoplasty, all incisions are made inside the nostrils. There is no visible scar from the outside. Because this method causes less disruption to the ligaments and the vascular-nerve structures at the nasal tip, it can be considered a more “conservative” approach. It may be preferred in patients who do not need major changes at the tip and who primarily have a hump problem. Recovery can be somewhat faster, and tip sensation often returns sooner.
In open rhinoplasty, a very small inverted-V incision is made on the area between the two nostrils called the “columella.” The nasal skin is fully lifted, and the framework is clearly exposed—like opening a car’s hood and looking at the engine. This technique provides the surgeon with exceptional visual control. Especially in difficult cases where the nose is very crooked, where there are significant asymmetries, or in revision cases, the open technique minimizes the margin of error.
So what about the incision scar? This is the biggest concern for patients. However, when sutured properly, this incision fades so much over time that it is almost impossible to see unless you get very close and look with a magnifying glass. Therefore, there is no such thing as “the best technique”; there is “the most suitable technique for your nose’s needs.” Your surgeon will decide which method will be safer and more effective based on your nasal anatomy.
What Are the Advantages of Piezo Surgery (Ultrasonic Rhinoplasty)?
In the past, the first image that came to mind when people thought of rhinoplasty was bruised eyes and a swollen face. The main reason for this was the use of crude tools like hammers and chisels to shape the bones. While breaking the bone, these tools could also damage surrounding vessels and soft tissues. Piezo technology—ultrasonic rhinoplasty—has completely changed this process.
Instead of breaking bones, the Piezo device uses very high-frequency sound waves to cut or rasp them as if drawing with a pencil. The most fascinating feature of this technology is that it is “selective.” In other words, the device is sensitive only to hard tissue like bone. Even if the tip accidentally touches the skin, a vessel, or a nerve, the device stops working as soon as it detects soft tissue and does not cause damage.
For the patient, the meaning of this precision is enormous. Because there is no soft tissue damage, postoperative bleeding is minimal, and bruising and swelling around the eyes drop to a minimum. Also, because we cut the bones in a controlled way, postoperative bony irregularities or palpable bumps are almost never seen. The main advantages Piezo technology offers are:
- Less bruising
- Less swelling
- Precise bone shaping
- Fast recovery
- Soft tissue protection
What Is Preservation Rhinoplasty?
In recent years, along with the trend of “returning to naturalness” in aesthetic surgery, a method has become popular: Preservation Rhinoplasty. In the traditional approach, to correct the hump, we would cut and remove the roof, then bring the side walls closer together to close the roof again. This is an effective method, but it could sometimes disrupt the natural curve of the nasal dorsum.
The philosophy of preservation rhinoplasty is based on the logic of “build without demolishing.” Here, we do not touch the roof of the nose at all, meaning the visible dorsum. Instead, by removing bone and cartilage from the base of the nose, we lower the entire nasal pyramid downward like an elevator. You can think of it like adjusting a tall building to the right height by lowering its foundation rather than shaving its floors from the top.
The biggest advantage of this technique is that the natural anatomy of the nasal dorsum is not disrupted. Light reflections and cartilage transitions remain completely original. Only the height of the nose decreases. This way, the nose looks much more natural after surgery and does not look “done.” In addition, because lymphatic channels and ligaments are preserved, the recovery process is surprisingly fast. However, not every nasal structure is suitable for this technique; especially in noses with very significant deviation, traditional methods may yield better results.
Get in Touch!
What Is the Postoperative Recovery Process Like?
When the surgery is over and you open your eyes, you will find a thermoplastic splint on your nose and silicone packs inside. Don’t let the word “pack” scare you. The old gauze packs that used to be meters long when removed are now history. The new-generation silicone packs are grooved in the middle, meaning you can breathe through these openings from the moment you wake up.
The first 2–3 days are the most challenging part of the process. Swelling in your face may increase, and your nose may feel blocked. To describe this feeling, think of the worst flu you have ever had: your nose is full, there is heaviness in your head, but there is no severe pain. Most of my patients do not even need painkillers. Cold application is your best friend during this period.
We usually remove the silicone packs on the 2nd or 3rd day. This takes seconds and is painless; the moment they come out, you experience the relief of taking a deep breath. At the end of the first week, we remove the cast on your nose. That moment is your first meeting with your new nose. But I must give you a warning: The nose you see is not your final result. It is still swollen, edematous, and the lines have not fully settled.
You can return to social life in the first weeks, but you must protect your nose like a baby. The nose taking its final shape is a long marathon. By the first month, the general shape becomes apparent; by the third month, details emerge; but full settling can take up to a year. The restrictions to pay attention to during recovery are:
- Heavy sports
- Wearing glasses
- Sun exposure
- Sauna
- Hot showers
- Impacts
Is There a Risk of Nasal Tip Drooping?
One of the biggest nightmares for patients is the nasal tip sagging downward months or years after surgery—“drooping.” Unfortunately, this is not an urban myth; it can occur as a result of technical insufficiency. Gravity, facial expressions, and the weight of the skin continuously pull the nasal tip downward. If the surgeon tries to keep the nose up only with sutures, those sutures can loosen over time and the tip may droop.
In modern surgery, we do not leave things to chance. We use “structural support” methods to keep the tip in place. You can think of it as the central pole of a tent. We place a strong piece of cartilage taken from inside the nose into the nasal tip like a column. This cartilage column (strut graft) physically prevents the nose from descending over time.
We also use special techniques that integrate the nasal tip into the septal cartilage. This makes the tip so stable that it does not bend even if you press on it with your finger, and it maintains its form. With correct techniques and sufficient cartilage support, the risk of tip drooping is extremely low. The tip settles only by a millimetric amount as postoperative swelling subsides, which is a natural process that we calculate and desire.
In Which Situations Is Revision Rhinoplasty Performed?
Sometimes, not everything may go exactly as planned. Rhinoplasty is performed on human tissue, and how that tissue will respond during healing is not always 100% predictable. According to global statistics, even the best surgeons have a revision (correction) possibility of 5–10%. Sometimes this can be a minor rasping procedure, and sometimes it may require reshaping the nose.
The reasons for revision vary. Sometimes dissatisfaction with the shape, sometimes persistent breathing problems, and sometimes deformities due to an impact can necessitate revision. However, it should be remembered that revision surgeries are technically more difficult than primary surgery. Because the natural anatomy inside has changed, tissues have adhered to each other (fibrosis), and cartilage reserves we can use have decreased.
If there is not enough cartilage left inside the nose, we may need to take cartilage from the ear or the rib to rebuild the nose. While this may sound a bit intimidating, rib cartilage allows excellent results because it provides strong and abundant material. The most important rule for revision is patience; at least one year should pass after the first surgery for tissues to soften completely and for blood circulation to return to normal. Common situations that require revision surgery are:
- Nasal tip drooping
- Insufficient hump reduction
- Difficulty breathing
- Irregularities on the nasal dorsum
- Asymmetries
- Imbalance in the nostrils